The management of spondylolisthesis, a condition characterized by the slipping of one spinal vertebra over the one beneath it, often raises questions about the necessity of surgical intervention. While severe cases might warrant such measures, the possibility of non-surgical treatments presents an engaging line of inquiry. Are physical therapy, strategic exercise, and pain management techniques sufficient in mitigating the symptoms and enhancing the patient’s quality of life? Could the answer lie in simple lifestyle modifications? This discussion calls for an in-depth exploration of these potential alternatives.
Understanding Spondylolisthesis
Spondylolisthesis, a medical condition often concealed by its complex name, involves the shifting of one vertebra out of line with the one below it. This malalignment can occur in any part of the spine, but it is most commonly seen in the lumbar region, which bears the majority of the body’s weight. The condition can result from congenital anomalies, degenerative changes, trauma or even repetitive strain injuries.
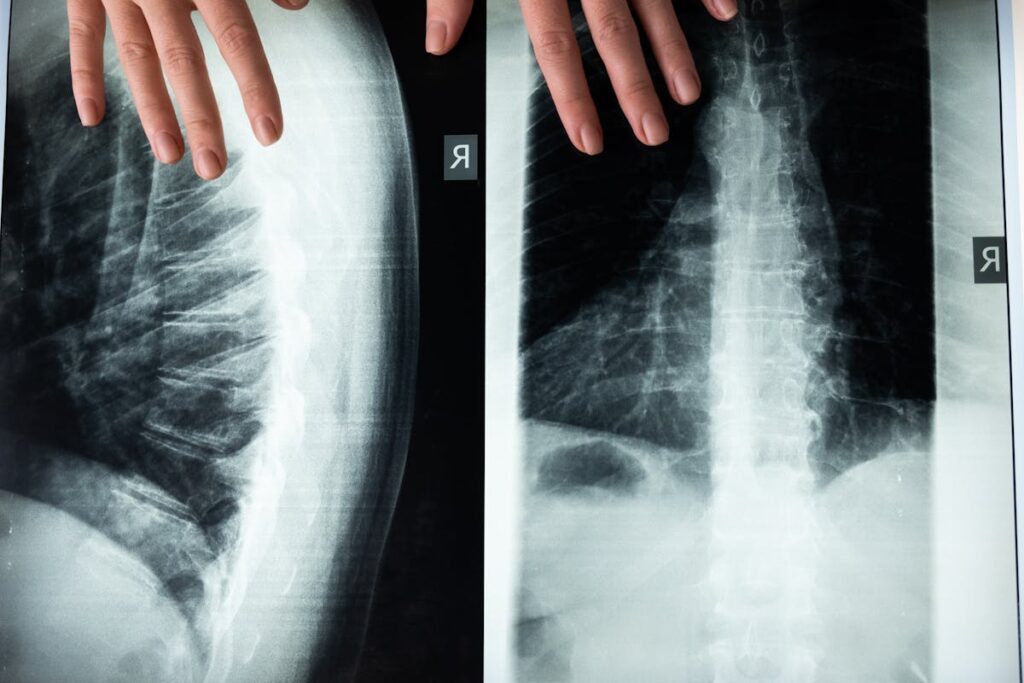
Diagnostic imaging plays a crucial role in the identification and classification of spondylolisthesis. X-rays, CT scans, and MRIs provide a detailed visual representation of the spine, enabling medical professionals to analyze the extent and direction of the slippage. It is also instrumental in ruling out other potential causes of back pain.
Patient education is a cornerstone in managing spondylolisthesis. Understanding the nature of the condition, its implications, and potential treatment options empower patients to make informed decisions about their care. It may also mitigate anxiety and encourage adherence to prescribed therapeutic regimens. A thorough understanding of spondylolisthesis, facilitated by diagnostic imaging and patient education, is fundamental to ensuring effective and individualized patient care.
Common Symptoms of Spondylolisthesis
While an extensive understanding of spondylolisthesis is the bedrock of managing the condition, recognizing the common symptoms is integral to early diagnosis and effective treatment. The presentation of this ailment varies considerably among patients, necessitating a thorough symptom assessment for an accurate diagnosis.
The most common symptom of spondylolisthesis is lower back pain, often radiating to the buttocks and down the legs. This pain typically exacerbates with physical activity and eases with rest. Patients may also experience muscle spasms, stiffness, and a sensation of tightness, particularly in the hamstrings. In severe cases, loss of bowel or bladder control may occur, signaling nerve damage.
Patient experiences can shed light on the severity and progression of the condition. While some patients may report consistent pain, others describe episodes of acute discomfort interspersed with periods of relief. Importantly, the degree of vertebral slippage does not always correlate with the severity of symptoms, underscoring the complexity of this condition.
Causes and Risk Factors
The onset of Spondylolisthesis can be attributed to a variety of causes, which we will explore in this section. It is essential to understand not only the common risk factors associated with the condition, but also the potential hereditary influences. This multi-faceted approach will provide a thorough view of the etiological factors related to Spondylolisthesis.
Understanding Spondylolisthesis Causes
In a significant number of cases, spondylolisthesis is a result of a congenital defect or an injury. This condition occurs when one of the vertebrae in the spinal column slips forward onto the bone below it. Understanding the causes of this disorder is essential for preventive and therapeutic purposes.
A genetic predisposition is one of the factors that often contribute to the development of spondylolisthesis. Certain individuals have weaker vertebrae due to inherited characteristics, making them more susceptible to this condition.
Furthermore, the mechanisms of injury play a vital role. High-impact sports or strenuous physical activities can cause undue stress on the lower back, leading to the displacement of vertebrae.
Other causes of spondylolisthesis include:
- Degenerative changes in the spine due to age-related wear and tear
- Infections that weaken the spine
- Tumors that disrupt the normal structure of the vertebrae
- Birth defects affecting the construction of the spinal bones
- Surgical procedures that inadvertently damage the spine
This holistic comprehension of the causes of spondylolisthesis is fundamental for the development of robust preventive strategies and efficient treatment options.
Common Risk Factors
How does one assess the potential risk factors for spondylolisthesis? Careful consideration of various elements such as age factors, activity levels, gender differences, obesity impact, athletic injuries, occupational hazards, and spinal alignment can help identify those at risk.
Age factors are significant in determining the likelihood of spondylolisthesis. As age increases, natural degeneration of the spine can lead to this condition. Activity levels also play an essential role. High-intensity activities or sports that involve heavy lifting or hyperextension can contribute to the onset of this condition, pointing to the role of athletic injuries.
Gender differences surface in the incidence of spondylolisthesis with females being more susceptible, primarily due to hormonal and anatomical differences affecting spinal alignment. Obesity exacerbates the strain on the spine, increasing the risk of spondylolisthesis. Similarly, occupational hazards associated with jobs requiring repetitive heavy lifting or long periods of standing can contribute to the condition.
While genetic predisposition is a significant factor, it is important to distinguish it from hereditary influences which will be discussed in the next segment. To summarize, understanding these risk factors is critical in the early identification and proactive management of spondylolisthesis.
Hereditary Influence on Spondylolisthesis
Tracing the roots of spondylolisthesis often leads us to hereditary influences. Numerous studies suggest a strong genetic predisposition to this condition, pointing to familial patterns that should not be overlooked. The genetic makeup of an individual can markedly influence the structural integrity of the spine, making some more susceptible to developing spondylolisthesis.
There several key factors related to hereditary influence on spondylolisthesis:
- Genetic variations: Certain genetic abnormalities can affect the spine’s structure and strength, increasing the likelihood of spondylolisthesis.
- Familial patterns: Observations show that spondylolisthesis often runs in families, indicating a likely genetic component.
- Congenital conditions: Some individuals are born with spinal abnormalities that can predispose them to spondylolisthesis.
- Ethnicity: Certain ethnic groups have been found to have a higher prevalence of spondylolisthesis, suggesting a genetic factor.
- Sex: Research indicates that women may be more genetically predisposed to develop spondylolisthesis than men.
Non-Surgical Treatment Overview
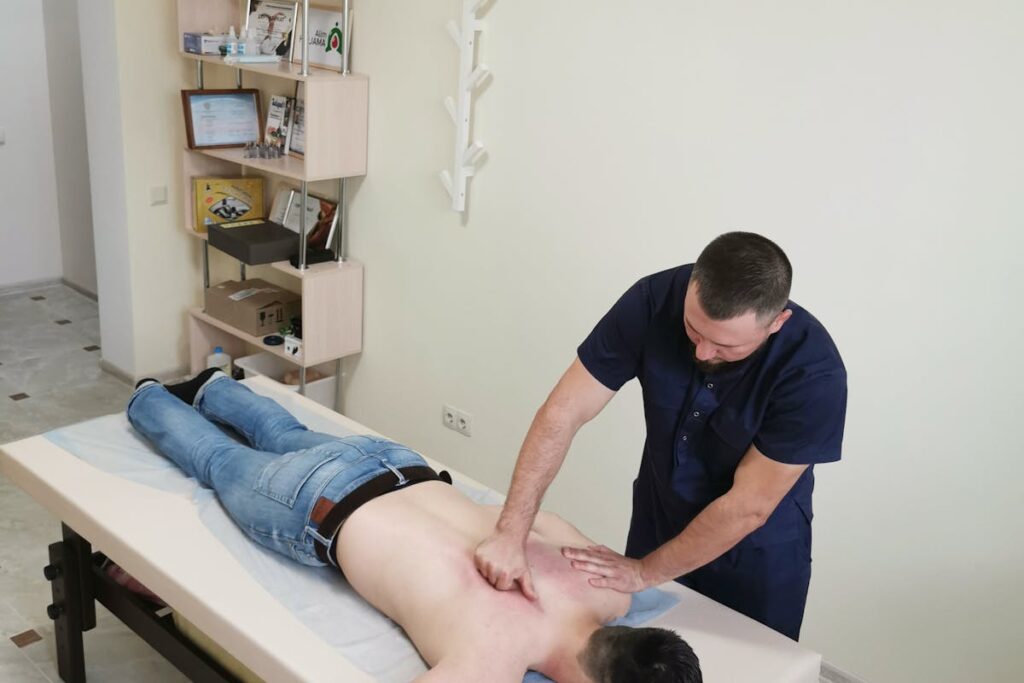
In managing spondylolisthesis, a variety of non-surgical interventions play pivotal roles. Physical therapy regimes, specifically tailored to individual patient needs, can greatly alleviate symptoms and enhance overall function. Concurrently, pain management techniques, including pharmacological and non-pharmacological strategies, are essential in mitigating discomfort and improving the quality of life for the patient.
Physical Therapy Approaches
Embracing a non-surgical route, physical therapy approaches serve as a key component in the treatment of spondylolisthesis. Physical therapists develop individualized exercise routines designed to mitigate discomfort, enhance mobility, and strengthen the muscles supporting the spine. These routines are usually a blend of stretching, strengthening, and low-impact aerobic exercises. Patient education is another pivotal aspect of this approach, ensuring individuals understand their condition, the objectives of their therapy, and how to perform exercises correctly to maximize benefits and prevent further injury.
These effective physical therapy approaches include:
- Tailored exercise routines focusing on core strengthening and flexibility
- Patient education on accurate exercise techniques and posture correction
- Use of heat and cold therapy to alleviate pain and inflammation
- Traction therapy, which can help to gently realign the vertebrae
- Manual therapy, where the therapist uses hands-on techniques to improve joint and soft tissue mobility
Pain Management Techniques
While physical therapy serves as a fundamental approach in managing spondylolisthesis, it is often paired with specific pain management techniques to optimize patient comfort and function. These techniques include but are not limited to, mind-body techniques and acupuncture. Additionally, consulting with an orthopedic spine specialist can provide further insights on personalized pain management strategies, especially for those experiencing radiating pain similar to sciatica.
Mind body techniques such as mindfulness, meditation, and biofeedback can be highly beneficial in pain management. These practices focus on developing patients’ ability to control their own physiological responses, which can help decrease pain perception, reduce stress, and promote relaxation. Regular practice can lead to notable improvements in coping with the chronic pain associated with spondylolisthesis.
Acupuncture, a staple in traditional Chinese medicine, has also proven to have considerable benefits in managing spondylolisthesis-related pain. By stimulating specific points on the body, acupuncture can help alleviate pain by releasing endorphins, the body’s natural painkillers, and by affecting the part of the brain that governs serotonin, a brain chemical involved with mood.
Each patient is unique, hence the effectiveness of these techniques will vary. However, when combined with physical therapy, these non-invasive pain management techniques can remarkably improve the quality of life for individuals dealing with spondylolisthesis.
Physical Therapy for Spondylolisthesis
Physical therapy plays an essential role in the thorough management of spondylolisthesis. It is an integral component of non-surgical treatment, aiming at reducing pain, improving function, and preventing further slippage. Therapists tailor programs to individual needs, often focusing on strengthening exercises and posture correction.
These are primary components of a physical therapy program for spondylolisthesis: * Strengthening exercises: Targeting the core and spinal muscles to provide better support and stability for the spine. * Posture correction: Teaching patients how to stand, sit, and move correctly to reduce pressure on the spine. * Flexibility exercises: Helping to improve the range of motion in the spine and alleviate muscle tension. * Pain management techniques: Incorporating heat or cold therapy, massage, and other non-pharmaceutical methods. * Education: Empowering patients with knowledge about their condition and how to manage it.
Through regular and consistent physical therapy, patients can often achieve significant improvements in their symptoms, reduce their need for pain medication, and possibly even avoid surgery. It is essential to follow the prescribed regimen diligently for optimum results. In some cases, additional interventions may be necessary, which will be discussed in the next section on “Medication Management”.
Medication Management
Maneuvering the complex landscape of medication management, patients with spondylolisthesis have several pharmaceutical options to help alleviate their symptoms. Initial treatment often involves over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs), like ibuprofen or naproxen. These medication types are primarily used for pain relief and inflammation reduction.
In cases where NSAIDs are ineffective, physicians might prescribe stronger pain relievers. Opioids, although potent, are used sparingly due to their potential for dependency and adverse side effects. Muscle relaxants can also be prescribed to help with muscle spasms often associated with spondylolisthesis.
Corticosteroids, either oral or injected, are another medication type used for their potent anti-inflammatory properties. Dosage guidelines for corticosteroids require careful management due to the potential side effects, including osteoporosis, hypertension, and susceptibility to infections.
Lastly, nerve pain medications, such as gabapentin or pregabalin, can be effective for patients experiencing radiating or nerve-related pain. These medication types are particularly beneficial when the spondylolisthesis affects nerve function.
It is essential for patients to adhere to the specific dosage guidelines provided by their healthcare provider to guarantee ideal effectiveness and to minimize potential side effects. Regular follow-ups and medication reviews are vital components of effective medication management for spondylolisthesis.
Lifestyle Modifications for Relief
In the journey towards managing spondylolisthesis, lifestyle modifications play an essential role in providing relief and slowing the progression of the condition. These modifications can be implemented independently, often without the need for medical intervention, and can considerably improve the quality of life for individuals suffering from this spinal disorder.
Fundamental lifestyle changes include dietary modifications and tailored exercise routines, both of which are instrumental in managing spondylolisthesis. Dietary changes help in mitigating inflammation and maintaining a healthy weight, thereby reducing the pressure on the spine. On the other hand, specific exercise routines strengthen the muscles supporting the spine, improving overall spinal alignment and stability. If you are also managing sciatica symptoms associated with spondylolisthesis, it may be beneficial to consider consulting an orthopedic spine specialist for personalized advice and treatment plans.
The following modifications, when incorporated into one’s daily routine, can provide substantial relief:
- Adherence to an anti-inflammatory diet rich in lean proteins, fruits, vegetables, and healthy fats to reduce inflammation and promote healing.
- Regular participation in low-impact exercises such as walking, swimming, or yoga.
- Avoidance of activities that put excessive strain on the spine, like heavy lifting.
- Consistent practice of good posture, both while standing and sitting.
- Regular check-ins with a healthcare professional to monitor the progress and make necessary adjustments.
Consequently, through disciplined lifestyle changes, it is possible to manage spondylolisthesis without resorting to surgical intervention.
When to Consider Surgery
Despite best efforts to manage spondylolisthesis through lifestyle modifications, there are circumstances when surgical intervention may become necessary. The decision to undergo surgery often hinges on the severity of the condition and the impact it has on a patient’s quality of life. Symptoms such as chronic pain, nerve compression, or progressive spinal deformity are indicators that surgical options may need to be considered.
There are various surgical options available, each with its own recovery timeline. These options range from minimally invasive procedures, such as laminectomy to remove bone spurs, to more complex surgeries like spinal fusion. The choice of procedure depends on the degree of vertebral displacement and associated complications.
The recovery timeline post-surgery is variable, typically ranging from a few weeks to several months. However, the primary goal of surgery is to stabilize the spine, relieve symptoms, and prevent further slippage, thereby improving overall life quality.
Frequently Asked Questions
What Is the Long-Term Prognosis for Individuals With Spondylolisthesis?
The long-term prognosis for individuals with spondylolisthesis varies, depending on severity and response to treatment. Patient experiences differ, but many report improved outcomes with sustained management of symptoms through non-surgical interventions like physical therapy and medication.
Can Spondylolisthesis Lead to Other Health Complications?
Yes, spondylolisthesis can lead to other health complications. Pain management becomes necessary due to chronic discomfort. Additionally, neurological issues may arise if the condition causes compression of spinal nerves.
Is Spondylolisthesis Hereditary?
Spondylolisthesis is not typically considered hereditary. However, genetic factors may predispose certain individuals to conditions that can lead to it, and familial patterns of spinal abnormalities have been observed in some cases.
Are Certain Sports or Physical Activities More Likely to Worsen Spondylolisthesis?
Certain sports and physical activities, particularly those involving hyperextension or high-impact movements, can exacerbate spondylolisthesis. An impact assessment and activity modification are recommended to minimize risk and manage the condition effectively.
Are There Any Alternative Therapies Available for Spondylolisthesis?
Yes, alternative therapies like chiropractic care and physical therapy can be effective in managing spondylolisthesis symptoms. These non-surgical treatments focus on strengthening the surrounding muscles and improving spinal alignment to alleviate discomfort.